- HYGEIA
- Vision & Mission
- Virtual tour
- Timeline
- Organizational structure
- Press Releases
- 50 Years HYGEIA
- Social responsibility
- Awards and Distinctions
- Human Resources
- Scientific & Training activities
- Articles – Publications
- Our Facilities
- Magazines
- Healthcare Programs
- Health Articles
- Financial Statements
- Doctors
- Services
- Medical Divisions & Services
- Imaging Divisions
- Departments
- Units
- Centers of Excellence
- Emergency – Outpatient
- Nursing Service
- Ambulances
- Cardiac Sector
- Maternity Clinic
- Baby’s Birth Registration
- Maternity Clinic Medical Services
- Paediatric Clinic
- Paediatric Clinic Medical Services
- Respiratory Conditions & Allergy Department
- Developmental Pediatrics Department
- Pediatric Imaging
- Pediatric Gastroenterology
- Pediatric Dermatology
- Electrophysiology Laboratory
- Electroencephalography for children
- 2nd Pediatric Cardiac Surgery
- Child & Adolescent Spine Center
- Hereditary Hemolytic Anemia
- Clinical Genetics
- Pediatric Craniofacial Surgery Department
- Cardiac MRI
- Sleep Study Center
- 1st Pediatric Neurosurgical Department
- 2nd Neurosurgical Department
- Pediatric Neurology
- 1st Pediatric Orthopaedics Department
- 2nd Pediatric Orthopaedics Department
- Pediatric and Adolescent Oncology
- Pediatric Urology Department
- Pediatric Ophthalmology
- Pediatric Infectious Diseases Department
- Child & Adolescent Endocrinology and Diabetes
- Clinical Pediatrics
- Child-Young Adult Gynecology
- Paediatric Cardiology & Adult Congenital Heart Disease Department
- Pediatric Nephrology
- Pediatric Plastic Surgery Department
- Pediatric Reumatology
- 1st Pediatric Surgery Department
- 2nd Pediatric Surgery Department
- 3rd Pediatric Surgery Department
- Children & Adolescents Mental Health Department
- 1st Otorhinolaryngology Department
- 2nd Pediatric Otorhinolaryngology Department
- Patients
HYGEIA
SERVICES
MATERNITY CLINIC
- Baby’s Birth Registration
Maternity Clinic Medical Services
PAEDIATRIC CLINIC
Paediatric Clinic Medical Services
- Respiratory Conditions & Allergy Department
- Developmental Pediatrics Department
- Pediatric Imaging
- Pediatric Gastroenterology
- Pediatric Dermatology
- Electrophysiology Laboratory
- Electroencephalography for children
- 2nd Pediatric Cardiac Surgery
- Child & Adolescent Spine Center
- Hereditary Hemolytic Anemia
- Clinical Genetics
- Pediatric Craniofacial Surgery Department
- Cardiac MRI
- Sleep Study Center
- 1st Pediatric Neurosurgical Department
- 2nd Neurosurgical Department
- Pediatric Neurology
- 1st Pediatric Orthopaedics Department
- 2nd Pediatric Orthopaedics Department
- Pediatric and Adolescent Oncology
- Pediatric Urology Department
- Pediatric Ophthalmology
- Pediatric Infectious Diseases Department
- Child & Adolescent Endocrinology and Diabetes
- Clinical Pediatrics
- Child-Young Adult Gynecology
- Paediatric Cardiology & Adult Congenital Heart Disease Department
- Pediatric Nephrology
- Pediatric Plastic Surgery Department
- Pediatric Reumatology
- 1st Pediatric Surgery Department
- 2nd Pediatric Surgery Department
- 3rd Pediatric Surgery Department
- Children & Adolescents Mental Health Department
- 1st Otorhinolaryngology Department
- 2nd Pediatric Otorhinolaryngology Department
- HYGEIA
HYGEIA
- Vision & Mission
- Virtual tour
Virtual tour
- Timeline
- Organizational structure
- Press Releases
- 50 Years HYGEIA
- Social responsibility
- Awards and Distinctions
- Human Resources
- Scientific & Training activities
- Articles – Publications
- Our Facilities
- Magazines
- Healthcare Programs
- Health Articles
- Financial Statements
- Doctors
- Services
Services
- Medical Divisions & Services
- Imaging Divisions
- Departments
- Units
- Centers of Excellence
- Emergency – Outpatient
- Nursing Service
- Ambulances
- Cardiac Sector
- Maternity Clinic
Maternity Clinic
- Baby’s Birth Registration
- Maternity Clinic Medical Services
Maternity Clinic Medical Services
- Paediatric Clinic
Paediatric Clinic
- Paediatric Clinic Medical Services
Paediatric Clinic Medical Services
- Respiratory Conditions & Allergy Department
- Developmental Pediatrics Department
- Pediatric Imaging
- Pediatric Gastroenterology
- Pediatric Dermatology
- Electrophysiology Laboratory
- Electroencephalography for children
- 2nd Pediatric Cardiac Surgery
- Child & Adolescent Spine Center
- Hereditary Hemolytic Anemia
- Clinical Genetics
- Pediatric Craniofacial Surgery Department
- Cardiac MRI
- Sleep Study Center
- 1st Pediatric Neurosurgical Department
- 2nd Neurosurgical Department
- Pediatric Neurology
- 1st Pediatric Orthopaedics Department
- 2nd Pediatric Orthopaedics Department
- Pediatric and Adolescent Oncology
- Pediatric Urology Department
- Pediatric Ophthalmology
- Pediatric Infectious Diseases Department
- Child & Adolescent Endocrinology and Diabetes
- Clinical Pediatrics
- Child-Young Adult Gynecology
- Paediatric Cardiology & Adult Congenital Heart Disease Department
- Pediatric Nephrology
- Pediatric Plastic Surgery Department
- Pediatric Reumatology
- 1st Pediatric Surgery Department
- 2nd Pediatric Surgery Department
- 3rd Pediatric Surgery Department
- Children & Adolescents Mental Health Department
- 1st Otorhinolaryngology Department
- 2nd Pediatric Otorhinolaryngology Department
- Patients
Sjögren’s syndrome
What is Sjögren’s syndrome?
Sjögren’s syndrome (pronounced Shurgren’s) is a condition which mainly affects the glands that produce saliva and tears, causing a dry mouth and/or eyes. The syndrome most commonly affects women aged 40–60.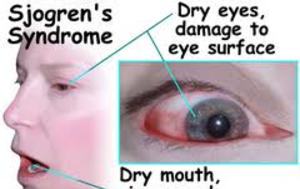
There are 2 types of Sjögren’s syndrome:
• primary – when it occurs on its own
• secondary – when it also occur in association with another rheumatic disease such as rheumatoid arthritis, lupus or scleroderma
It’s estimated that many people may be affected by Sjögren’s syndrome, but the exact figures aren’t known because many people never see a doctor about their symptoms.What are the symptoms of Sjögren’s syndrome?
Symptoms include:
• dry, sore, irritable or gritty eyes
• a dry mouth and/or throat, which may cause difficulty chewing or swallowing food
• tiredness (fatigue)
• joint pain or general achiness
You may also experience dryness of the skin, digestive tract, vagina or air passages.Other possible symptoms include:
• headaches
• fever
• swollen lymph glands in your neck, armpits or groin
• aggravated menopausal symptoms
• your fingers or toes turning blue in the cold (Raynaud’s phenomenon)
Sjögren’s syndrome can sometimes cause problems with your nervous system, liver and kidneys, inflammation of your blood vessels and chest pain.
Many people don’t have any other symptoms, but the range and severity of symptoms can vary a great deal from person to person.Eye problems
Your eyes may be dry and feel sore, irritable or gritty. Some people find strong lights can be uncomfortable, while others find their eyes become sticky with mucus.Mouth and throat problems
Your mouth may become dry and you may have mouth ulcers, which can sometimes cause a sticky feeling in your mouth or throat. It may be difficult to swallow and your sense of taste may be altered. Your voice may be hoarse or weak, and some people have a dry cough.
Occasionally a very dry mouth can lead to other problems such as fungal infections (e.g. thrush), an unpleasant taste in your mouth and increased dental decay. Your salivary glands may also become painful and/or swollen.Extreme fatigue
Fatigue (extreme tiredness) is one of the most common symptoms, and it can’t be cured by a good night’s sleep. Some people may also feel down or depressed.Aches and pains
Your joints may be painful and swollen due to inflammation, while some people have a general achy feeling or tenderness at various points around their body. Joint problems are usually less severe than in conditions such as rheumatoid arthritis.Other symptoms
Other parts of your body may also be drier than normal, for example:
• your digestive passage, making it difficult to swallow food
• your bowel, causing symptoms similar to irritable bowel syndrome (e.g. abdominal pain)
• your vagina, making sex uncomfortable
• your skin, which may also be itchy or unusually sensitive to strong sunlight
• your air passages, making you more sensitive to irritants such as smoke or dustOther problems and complications that can sometimes be associated with Sjögren’s syndrome include:
• fever
• cold, blue fingers (Raynaud’s phenomenon)
• migraine-like headaches
• swollen lymph glands in your neck, armpits or groin
• aggravated menopausal symptoms
• problems with your nervous system, such as weakness or numbness
• inflamed blood vessels (known as vasculitis)
• chest pain (caused by pleurisy) or breathlessness
• liver or kidney problemsWho gets Sjögren’s syndrome?
Women aged between 40 and 60 are most likely to be diagnosed with Sjögren’s syndrome. Only about 1 in 10 Sjögren’s syndrome patients are men, and the condition only rarely occurs in childhood.
It’s possible that some people are more likely to get Sjögren’s syndrome because something in their genes makes it difficult for them to get rid of certain infections. However, it’s unusual for children to inherit the condition from their mother or father.How is Sjögren’s syndrome diagnosed?
Your doctor will ask about your symptoms and carry out tests to assess how dry your eyes and mouth are. You may also need to see an eye specialist (ophthalmologist), a dentist or oral surgeon, or a rheumatologist before you’re diagnosed.
What tests are there?
• Tear production – a small piece of sterilized, pre-packaged blotting paper is used to measure your tear production. This is called Schirmer’s test. The paper is placed in the corner of your eye and folded over your lower eyelid. This is a little uncomfortable and causes your eyes to water, making the paper wet. The amount of water that soaks into the blotting paper within 5 minutes is measured, and this tells the doctor how good your tear production is.
• Eye examination – an eye specialist will put a dye into your eyes and use an instrument called a slit lamp to examine them. The lamp shines a beam of light through a narrow slot and magnification allows the doctor to examine the surface of your eye more effectively. This makes it possible to see the film of liquid over the surface of each eye. If you don’t have enough of this liquid, it could be a sign that you have Sjögren’s syndrome.
• X-rays of your salivary glands and ducts (sialography) – rarely used.
• Other scans – ultrasound scans of the salivary glands or MRI scans.
• Blood tests – Complete blood count, ESD, CPR and urine tests, as well as special immunological tests.
People with Sjögren’s syndrome often have high levels of antibodies in their blood. Two particularly important antibodies are called anti-Ro and anti-La antibodies, which can also be seen in patients with lupus erythematosus. If you have anti-Ro and/or anti-La antibodies along with dry eyes and/or a dry mouth, it’s very likely that you have Sjögren’s syndrome.
Patients with Sjögren’s syndrome often have very high ESR levels regardless of whether they feel well or ill, unlike people who have other conditions such as systemic lupus erythematosus or rheumatoid arthritis. Measuring the ESR isn’t a good way to tell how active your condition is, so other measurements such as C-reactive protein (CRP) are better because they only rise when Sjögren’s syndrome becomes more active.
• Lip and salivary gland biopsy – several tiny salivary glands may be removed from your lower lip under a local anesthetic and examined under a microscope. This is usually only done if the diagnosis is still uncertain after the other tests. Further specialized tests may be needed if you develop swelling in your lymph glands (in the neck, armpits or groin) or if you have complications involving your chest, kidney, liver or nervous system.
Note that dry eyes and dry mouth may be due to other causes, such as
• dryness syndrome (the glands do not produce enough saliva or tears) – it develops later in life
• other conditions apart from Sjögren’s syndrome, such as sarcoidosis, which affect the lachrymal of salivary glands
• some drugs, such as antihistamine or antidepressants
• inflammation of the sebaceous glands of the eyelids (blepharitis), which causes excessive evaporation of the tear film
You must visit your doctor to be diagnosed. Your doctor will ask about your symptoms and perform tests to assess the dryness of your eyes and mouth.What treatments are there for Sjögren’s syndrome?
Although there’s no cure yet, many treatments are available to help your symptoms. These include:
• eye drops and ointments
• mouth gels and sprays, chewing gums or lozenges that increase saliva production
• painkillers and non-steroidal anti-inflammatory drugs (NSAIDs)
You may be prescribed other drugs, depending on the type and severity of your symptoms. Occasionally, a minor surgical procedure may be used to reduce the drainage of fluid from your eyes.Eye treatments
For dry, sore or irritable eyes:
• You can use lubricant eye drops several times a day.
• If you need eye drops more than 6 times a day, you should use a preservative-free formulation because frequent use of drops containing preservative can increase dryness and sensitivity. Preservative free formulations can be used up to hourly if you need to.
• For very dry eyes, you may need to use ointments (for example cyclosporine) or hyaluronate preparations.
If mucous and debris are causing stickiness:
• Mucolytic agents, such as acetylcysteine eye drops may be helpful.
• Paraffin-based ointments can be used at night if your eyes are dry and crusty when you wake up.
If you have corneal ulcers (severe pain in the eye accompanied by photophobia and redness) or infections, you should NOT use any of these treatments and should seek advice from an eye specialist. In some cases, an eye specialist may suggest punctal occlusion.
If your Sjögren’s syndrome is so bad that you have minimal tear production, punctal occlusion won’t help you. If your eyes remain very dry, your puncta may be sealed by cauterization.Mouth and throat treatments
For a dry mouth:
• Artificial saliva, such as gels, can be helpful.
• If you have your own teeth, fluoride mouth sprays are recommended because they may protect you against dental decay.
• If you’re able to produce some saliva, you can take pilocarpine as a tablet (Salagen). This works by stimulating glandular tissue. Some people may notice side-effects such as sweating, flushing, a change of bowel habit or a more frequent need to urinate. These effects usually ease after a time, and it may help to start on a low dose and gradually increase it as the side-effects decrease.
• If your mouth is severely dry and is causing other problems such as fungal infections or dry coughs, your doctor may recommend an antifungal treatment such as nystatin.
• Chlorhexidine mouth rinses may help with dental hygiene, and you can use fluoride mouthwashes or high concentration fluoride toothpastes to help reduce dental decay. Non-sugar chewing gum or other dental care products or lozenges can also help.For mouth ulcers:
• Triamcinolone acetonide ointment can be applied to mouth ulcers. If this doesn’t help, your doctor may prescribe corticosteroid pellets for you to keep in your mouth a few times a day.
• Oral rinses or sprays can help relieve discomfort from mouth ulcers.
• If the ulcers are causing stickiness in your mouth or throat, a diluted chlorhexidine mouthwash will help. Alternatively you could try rinsing and gargling with a mouthwash made from a mixture of a teaspoon of salt, a teaspoon of baking powder and a liter of water.
If your salivary glands are painful, ask your doctor for further assessment and advice – they’ll check whether you have an infection. If your salivary glands aren’t infected, they may prescribe a short course of a corticosteroid (prednisolone).Other treatments
Joint pain, aching or tender spots:
• Painkillers such as paracetamol and/or non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen may help.
• If your joints are inflamed, your doctor may suggest you have an intramuscular steroid injection or a short course of steroid tablets for short-term relief.
• Hydroxychloroquine can be used for longer term treatment (from 6 months to many years).
Extreme tiredness, lethargy, difficulty in concentrating:
• Your doctor may suggest blood tests to check your thyroid gland and to screen you for celiac disease.
• Hydroxychloroquine may help with fatigue and joint pain.
• Lifestyle changes, such as taking sensible exercise and pacing yourself in your daily activities, can also be helpful.Fever: Your doctor will want to rule out more serious problems, such as infection, thyroid problems or lymphoma.
Raynaud’s phenomenon:
Self-help measures like wearing an extra pair of socks or gloves, will often improve your symptoms, but drugs such as nifedipine, which open up the blood vessels, may be prescribed if necessary.Migraine-like headaches:
Painkillers or specific anti-migraine medications are usually effective.Abdominal pain, irritable bowel syndrome:
Antispasmodic drugs, such as mebeverine (Duspatalin) can be helpful for disrupted bowel habits.Aggravated menopausal symptoms:
Hormone replacement therapy (HRT) can be used if necessary, but it’s important to discuss the risk of side-effects with your doctor.If you have a more severe form of the condition or if your peripheral nervous system is affected you may need other medications, including:
• high-dose cortisone
• cyclophosphamide
• painkillers, including gabapentin or pregabalin, for nerve pain
• rituximab
• mycophenolateThe majority of people don’t need these drugs because their symptoms mostly affect their eyes and mouth.
Mild liver abnormalities aren’t common and probably won’t need treatment, but you should have regular checks. You may need specialist treatment if you develop a condition called primary biliary cirrhosis.Your lungs can occasionally be affected by fibrosis, which can cause breathlessness, a dry cough and chest pain. You’ll need specialist advice if you have fibrosis, but your doctor will be able to prescribe cortisone for it.
Self-help and daily living
Try the following self-help tips:
• Increase the humidity in rooms by introducing humidifiers, plants or bowls of water.
• Always have some water to hand.
• Follow a good dental routine and have regular check-ups.
• Increase the amount of fiber in your diet if you have bowel symptoms.
• Don’t have too many sugary or caffeinated foods and drinks.
• Use lubricating gels if sex is painful.Some symptoms of Sjögren’s syndrome can be eased by simple self-help measures:
• Wear wraparound sunglasses or glasses with side shields to help keep moisture in your eyes.
• Keep your eyelids and the surrounding areas clean to maximize oil secretion from glands in your eyelids.
• Avoid contact lenses because they’ll be uncomfortable if your eyes are dry.
• Consider wearing tinted glasses if you find strong lights uncomfortable.
• Increase the humidity in your home. This can help eye symptoms and a dry cough. Humidifiers, large-leaved houseplants or bowls of water all help to increase humidity in a room.
• Avoid strong soaps if you have dry, itchy skin. Water-based creams and emollients may be helpful.
• Wear sunscreen (factor 15 or higher) if your skin is sensitive to the sun or comes out in a rash.
• Wear warm gloves if you experience Raynaud’s phenomenon. Exercise will help by improving your circulation, but you should avoid smoking because it’s bad for the circulation.
• Good dental hygiene is recommended for any oral symptoms.
• Only take medications such as antibiotics if it’s really necessary as Sjögren’s syndrome can slightly increase the risk of side-effects. It’s important to have a good dental care routine and regular check-ups if you have oral symptoms of Sjögren’s syndrome.Exercise
You should exercise to keep mobile, particularly if you have symptoms in your joints. You’ll need to find the right balance between rest and exercise, especially if you also suffer from extreme tiredness. A physiotherapist will be able to give you advice on suitable exercises and increasing your activity level gradually.Diet and nutrition
No special diet is recommended for Sjögren’s syndrome, but increasing the amount of fiber in your diet should help if you have abdominal pain or bowel problems. Cutting down on sweet food and drinks will reduce your risk of dental problems.
Remember that alcohol, tea, coffee and other caffeinated drinks can be dehydrating. Sipping water or sucking ice cubes regularly can help to relieve the discomfort of a dry mouth.
Read more about diet and arthritis.Complementary medicine
There isn’t scientific evidence that suggests any specific complementary medicine can ease the symptoms of Sjögren’s syndrome.
If you have Raynaud’s phenomenon, vitamins E and C, evening primrose oil, fish oils and ginger or Ginkgo Biloba can also help.Sex and pregnancy
One less common symptom of Sjögren’s syndrome may be that you have a dry vagina, which can make sex painful. Lubricants should help and so can estrogen creams.
Treatments for infections such as thrush are readily available from chemists.
People with Sjögren’s syndrome don’t usually have any increased problems during or after pregnancy. In about 2% of women who have anti-Ro and/or anti-La antibodies, these antibodies are passed on to the baby during pregnancy and cause symptoms in the baby after birth. These symptoms can include rashes and abnormal blood tests, but both settle within a few weeks to a few months as the mother’s antibodies are gradually lost from the baby’s blood. In some cases the antibodies affect the baby’s heart, causing it to beat slowly.Remember that 98% of mothers with anti-Ro and anti-La have no problems with pregnancy, but if you know you have these antibodies you should mention this to your obstetrician because your baby’s heartbeat may need additional monitoring in the womb.
© 2007-2026 HYGEIA S.M.S.A. | ΓΕΜΗ: 000279901000Ο ιστότοπoς μας χρησιμοποιεί cookies για να καταστήσει την περιήγηση όσο το δυνατόν πιο λειτουργική και για να συγκεντρώνει στατιστικά στοιχεία σχετικά με τη χρήση της. Αν θέλετε να λάβετε περισσότερες πληροφορίες πατήστε Περισσότερα ή για να αρνηθείτε να παράσχετε τη συγκατάθεσή σας για τα cookies, πατήστε Άρνηση. Συνεχίζοντας την περιήγηση σε αυτόν τον ιστότοπο, αποδέχεστε τα cookies μας.
Αποδοχή όλων Άρνηση όλων ΡυθμίσειςCookies ManagerΡυθμίσεις Cookies
Ο ιστότοπoς μας χρησιμοποιεί cookies για να καταστήσει την περιήγηση όσο το δυνατόν πιο λειτουργική και για να συγκεντρώνει στατιστικά στοιχεία σχετικά με τη χρήση της. Αν θέλετε να λάβετε περισσότερες πληροφορίες πατήστε Περισσότερα ή για να αρνηθείτε να παράσχετε τη συγκατάθεσή σας για τα cookies, πατήστε Άρνηση. Συνεχίζοντας την περιήγηση σε αυτόν τον ιστότοπο, αποδέχεστε τα cookies μας.

- Paediatric Clinic
- Paediatric Clinic





































